Sepsis is on the minds of many physicians and laboratory directors in acute-care settings. It’s no wonder: Delays in the recognition and timely treatment of sepsis can have devastating consequences for patients and their families, and it can place a significant financial burden on healthcare institutions.
What makes the threat of sepsis so concerning to healthcare providers? It’s a time-critical condition, and when it comes to patient survival, every minute matters. Sepsis is also a condition that can sometimes hide in plain sight, leading to unnecessary delays in diagnosis and treatment.
The Challenge of Sepsis Diagnosis
While nearly every healthcare provider on the frontlines understands what sepsis is—a dysregulated immune response to infection characterized by systemic inflammation—it remains a confounding condition to diagnose.
First, the symptoms at presentation of sepsis may be vague. Approximately 30% of patients with sepsis present with non-specific symptoms;1 some patients may even lack typical symptoms of infection such as fever. It may take several hours for more conclusive evidence of sepsis—such as organ dysfunction—to appear.2 The emergence of organ dysfunction defines severe sepsis under the Sepsis-2 definition and sepsis under the Sepsis-3 definition, and the risk of death increases for these patients.
Second, diagnostic criteria for sepsis comprise vital sign measurements including heart rate, respiratory rate, body temperature (fever) and, often, an evaluation of mental status. The first three criteria allow for an assessment of what is referred to as Systemic Inflammatory Response Syndrome (SIRS), and the latter is part of the quick Sequential Organ Failure Assessment (qSOFA). Even still, whether a patient should be considered septic without clear evidence of organ dysfunction is subjective, and studies have demonstrated a high level of discordance among physicians who encounter sepsis in regular practice.3 Even with guideline criteria like SIRS and qSOFA, two physicians evaluating the same patient may make different diagnoses.
Finally, the only diagnostic test that can answer the question, “Is it sepsis?” is a blood culture, which has limitations and is often negative, complicating diagnosis for patients undergoing that test. In fact, there are over 178 assays available commercially for sepsis, and all have limitations, particularly for less severely affected patients who do not exhibit organ dysfunction.4 That’s because sepsis is a syndrome with a complex pathobiology, and no test available today has sufficient sensitivity and specificity to conclusively point to it.
Delayed Sepsis Diagnosis: One Young Man’s Story
Manny Careaga was a healthy young man when he suddenly fell ill after a meal. Manny’s mother, Diana Careaga, brought him to the hospital. Doctors initially diagnosed Manny with appendicitis and dehydration. However, he wasn’t responding to typical treatments. Growing concerned, doctors kept Manny in the hospital overnight.
What came next shocked his family and physicians: X-rays revealed Manny had an abscess the size of a soccer ball in his abdomen. Unbeknownst to his family and healthcare team, Manny’s body had been fighting a dangerous infection, which caused the development of a large pocket of pus within his abdomen. He underwent a needle aspiration, and eventually made a full recovery.
Like a subset of patients with sepsis, Manny’s symptoms were not typical. He never experienced a fever, a hallmark symptom. His treating doctors attributed his symptoms to other causes. It wasn’t until another set of physicians reviewed his records that appropriate diagnosis and treatment occurred.
“He was such a healthy young man. It got to the point that it got to only because it was not identified early enough,” his mother recalls.
The Consequences of Delayed Sepsis Diagnosis
Prematurely discharging a patient with an infection from the emergency department (ED) to their home can lead to a repeat visit to the ED, often after the patient’s condition has deteriorated. This can reduce value-based reimbursements, as well as lead to higher costs for subsequent care in the future. Published research shows that the cost to treat patients with sepsis who are discharged to their home can be five times more than the cost to treat patients treated in the intensive care unit.5
The mortality rate of patients improperly dispositioned from the ED also rises. Mortality is approximately 30% for patients who are discharged properly diagnosed and transferred to the ICU and rises to 62% for those who are discharged to home.6
Mortality Rate for Patients Based on Discharge Location
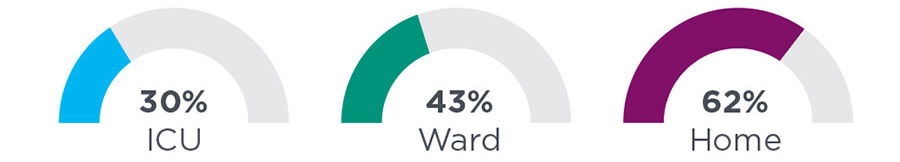
Figure 1. The rate of mortality for patients with or at risk of sepsis is highest when they are discharged to home.
Statistics, however, don’t tell the full story. A delayed sepsis diagnosis can have a devastating effect on the lives of patients and their families. Consider these stories of lives touched by sepsis:
- A 5-year old girl lost her battle to sepsis after multiple visits to doctors and the ED led to multiple misdiagnoses. The hospital ended up paying $4 million and new legislation regarding sepsis reporting was enacted in her name7
- A pregnant woman underwent three amputations, lost her sight and spent years in rehabilitation after contracting streptococcal pneumonia that led to sepsis8
- A newly married mom to a baby boy died after the flu left her with secondary sepsis that went undiagnosed, even after 15 hours in the hospital9
Helping Clinicians Address Sepsis
Advancements in early sepsis detection and diagnosis are on the horizon. Someday, clinicians may be able to leverage artificial intelligence and machine learning algorithms to detect sepsis. By combining novel laboratory tests with electronic health record information, the hope is that these algorithms could accurately predict and detect sepsis earlier, with the goal of reducing mortality and the cost of care through earlier intervention.
A novel biomarker is also being recognized for its promise as an aid in improving early sepsis detection. Monocyte distribution width (MDW) is a statistical measure of the size distribution of monocytes. Monocytes are a type of white blood cell that become activated in infection and inflammation. This value can be obtained at the same time as a typical complete blood count (CBC), a common test administered to patients entering the ED. A multicenter trial validated monocyte distribution width as a novel indicator for Sepsis-2 and Sepsis-3 in high-risk emergency department patients.10
Could MDW aid your physicians in the diagnosis and risk stratification of sepsis?

 English
English